“Half this game is 90% mental.” – Yogi Berra.
We have had two homes actually.
Pete and I have been at his sister’s home intermittently for the last two months. (His knee injury occurred on 6/23.) Imagine the challenges we would have faced if we didn’t have our loving family nearby! We have managed to rearrange their living room (turning it into Pete’s bedroom), monopolize their downstairs bathroom, use the laundry facilities, add to the grocery bill and accidentally run over a flower bed. Abby and Maggie have given up their rooms for me. Helen, acting as concierge, has anticipated our needs. I credit her with clairvoyance. We’ve been made as comfortable as possible, as if this home was our own. We are so very grateful for Helen and Greg’s love and resources.

Our second home has been Hartford Hospital. After two inpatient visits and three procedures, we thought we were done with this institution. We thought we’d be cleared for travel at our office visit with Dr. O’Connor (7/25). Instead, we both cringed at the suggestion of a third wound irrigation. Admittedly, the lower end of the left knee incision still was not healing well, so we drove directly from the office visit to the hospital for what was expected to be an overnight stay. Instead, the Infectious Disease doctor had a “gut feeling” that something else was causing Pete’s ongoing low grade fevers and vague abdominal pain. The Abdominal CT (7/26) showed diverticulitis with an abscess. The next 15 days were a blur. I won’t describe the details, but I can say that “we have lived at Hartford Hospital,” and I have some insights to share.

We have a love-hate relationship with Hartford Hospital. We loved the new building (BJI), the valet parking, the clean and spacious rooms, the flat screen TVs, the complimentary WiFi, room service, friendly staff, and lovely picture window views. We loved knowing that this hospital has won awards left and right for excellence. We felt confidence in the fact that, as a teaching hospital, we were surrounded by brilliant minds and innovative thinking. We were not so fond of the parade of caregivers, providing bonafide caregiving, but frequently interrupting Pete’s restorative sleep. We grew tired of the many alarms associated with the medical devices and patient safety equipment, the overhead paging, and the chatter of staff members that passed by our doorway. Even the noise of the floor cleaning machine became annoying. We tolerated the various students, interns, residents and “attendings” asking many of the same questions day after day. Each team (orthopedic and surgical) and each shift would do their patient assessment, exposing body parts that are normally covered up, and poking areas that were known to be tender.
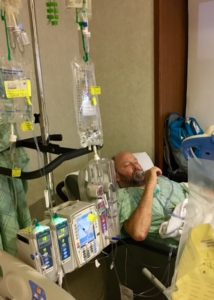
Our day started around 5:30 a.m., but it didn’t really have an ending. We had a caregiver of some kind in the room nearly every hour, sometimes several in the hour, including night shift. I spent my career in healthcare and I never realized how exhausting it is to be on the receiving end of care. Granted, Pete’s condition was serious for a spell, but it took tears and desperation to request “coordinated care” whereby the caregiving team could complete their work together, minimizing bedside time, allowing for patient rest. I had a couch or reclining chair in his private room and I spent all but one night with Pete, so I can attest to the challenges he/we faced.
With our third hospitalization, Pete and I were gaining notoriety. I developed a friendship with Carol, the Nurse Director of the Bone and Joint Institute, early in Pete’s second inpatient stay. She was my lifeline. I didn’t really use it, but I knew I could. As a representative for hospital administration, she let me know that I was a “Partner in Care,” that I was not just the wife of a patient, a passive bystander, but that my presence counted, my opinions and insights were important, and that I could contact her directly for any concerns. This gave me great comfort.

When we transferred from BJI to “Bliss 8” (the surgical floor in a different building), Carol greased the wheels and made sure that the new unit Nurse Director (Susanne) knew our story. She advocated for a private room (so I could stay the night) and she visited almost daily. Her friendship and encouragement helped me cope with my fatigue and what seemed like endless hours of emotional assault. In addition, Pete’s sisters were present and/or in regular contact boosting our spirits and providing me respite. We also reached out to God to get us through this painful and life-altering ordeal. He came through, as He always does.
We’re back at Helen’s, continuing with rehabilitation and learning the logistics of our new normal. We have an enlightened respect for health and healthcare. I have promised Carol that I will pen an article on our experience as care receivers, from the perspective of caregivers. I will also catch up on sleep!

Thanks for your thorough update, Susan – you’ve both been on my mind and of course in my prayers. Am glad for your excellent doctor who followed his gut feelings and that, in spite of all of it, you’re coming out the other side of this.
Blessings to you both as you rest at Helen’s – if this had to happen while out on the adventure, it couldn’t be in a better place!
Thankful for God’s faithfulness –
Kathy
Thank you for the courage and the strength to have kept (and keeping) going so you both can continue to inspire us! I as well have been sitting by the bed of the one that I love and was surprised at how difficult it was to be on “the other side” of caregiving…exhausted & scared to death, trying to be brave. I felt the same way about the floor cleaners! You are both loved deeply and I am so happy, finally, that you are on the road to recovery! Hurry home!
Susan, What a different summer you have had from what you had planned. There is a reason, we may not know it yet but God will use this experience for His Glory. Your strength and positivity are a credit to Him and a blessing to those around you and who read your words. We are praying for you, Pete, and your healthcare professionals. Be WELL, both of you!
Jean and Jerry
Aboard Makin Memories in Ontario (You will LOVE it here next year!)
So glad you guys have been able to get out and breathe the air and feel the sun. Wishing for a slow and steady growing strength so you can both get home. Your bed will never feel so good. Looking good, Pete.